GRACE KAEMPER
BVScV student
INTRODUCTION
Hemipelvectomy is a surgical procedure involving removal of the hemipelvis and corresponding hindlimb. It can be classified as total or subtotal, where subtotal has three further subtypes: mid-to-cranial, mid-to-caudal and caudal (Barbur et al. 2015).
There is a paucity of veterinary literature detailing both technical and clinical aspects of hemipelvectomy. One study presents hemipelvectomies as “complex, aggressive surgical procedures” with a high risk of intraoperative complications and “a slower return to ambulation than amputation” (Kramer et al. 2008). There is a need to challenge this commonly held perception in the veterinary industry, and the purpose of this case report is to present hemipelvectomy as a viable treatment option for a range of otherwise inaccessible tumours.
This case study examines three dogs that underwent hemipelvectomy in 2018 at a single veterinary specialist hospital in Auckland. Two dogs presented with osteosarcoma of the proximal femur and ilium respectively, and the third was diagnosed with a peripheral nerve sheath tumour (PNST) of the sciatic nerve. In all three cases, the location of the tumour rendered standard limb amputation (coxofemoral disarticulation) insufficient for primary tumour control. Therefore, a hemipelvectomy was required to obtain appropriate surgical margins.
All dogs were followed from diagnosis and surgery, through to recovery, to examine both the oncologic and functional outcomes. See Table 1 for a summary of the three cases.
CASE ONE
A 13-year-old, female, spayed Labrador Retriever presented with acute left hindlimb lameness of 10 days’ duration. Radiographs revealed a pathological fracture of the proximal left femur with suspected neoplastic involvement of the ipsilateral coxofemoral joint. Thoracic radiographs showed a 5 mm-diameter, rounded, soft-tissue nodule in the caudodorsal aspect of the right caudal lung lobe. Definitive tissue sampling of the pulmonary nodule was not obtained, and both benign and malignant considerations were given during clinical decision making. An abdominal ultrasound identified a bilobed, diffusely heterogenous, soft-tissue mass of 31 mmx 12 mm effacing the left adrenal gland, and mild left medial iliac lymphadenopathy. Preoperative biopsy of the fracture site was not pursued, as treatment was with palliative intent.
A subtotal mid-to-cranial hemipelvectomy with concurrent amputation of the left pelvic limb was performed, utilising an osteotomy of the ilium caudal to the sacrum, osteotomy of the pubis within the obturator foramen, and osteotomy of the cranial ischium. Soft tissue dissection was performed outside the muscular compartment containing the fracture, such that the fracture haematoma and tumour were not encountered during surgery. Haemostasis was achieved with an electrothermal vessel sealing device (Ligasure; Medtronic Corporate ANZ, Auckland, NZ) and no complications arose during surgery.
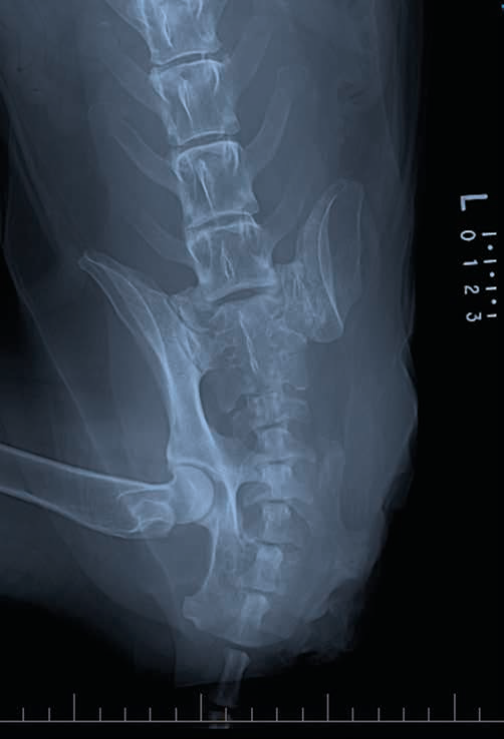
Fig.1 Dorsoventral radiograph of the pelvis of a Labrador Retriever taken 10 weeks after hemipelvectomy surgery as palliative treatment for osteosarcoma of the left proximal femur and acetabulum. There is an aggressive monostotic lesion of the right ischium with motheaten lysis, heterogenous sclerosis and irregular periosteal new bone formation.
Histopathology identified the proximal femoral/acetabular malignancy as an osteosarcoma with haemorrhage and necrosis. Surgical margin assessment revealed no neoplastic cells within 40 mm of the inked margins.
The dog was strongly ambulatory following surgery and was discharged from hospital the day following her hemipelvectomy. The functional outcome, as reported by the owner, was excellent for 10 weeks after surgery. At that time, the dog developed acute non-ambulatory paresis and urinary incontinence. Neurologic examination was consistent with a painful L7-S3 lesion. Radiographs revealed motheaten lysis and heterogeneous sclerosis of the right ischium, and further pulmonary nodules (Figure 1). Advanced imaging and tissue biopsy were declined, but distant metastasis (spine and lungs) was suspected. The dog was discharged with analgesia provided by 400 mg gabapentin (Neurontin; Pfizer New Zealand, Auckland, NZ) and 37.5 mg carprofen (Rimadyl; Zoetis New Zealand Ltd, Auckland, NZ) both given orally twice daily, but was euthanised due to lack of clinical improvement.
CASE TWO
An 11-year-old, male, neutered Staffordshire Bull Terrier presented with acute, weight-bearing lameness of the left hind limb of 10-days duration. Pain and soft-tissue swelling in the region of the left ilial body; a rectally palpable ilial mass; and atrophy of the left gluteal and quadriceps muscles were identified. Incisional biopsy of the soft-tissue component of the mass was consistent with osteosarcoma of the left ilial body. Staging using computed tomography (CT) of the thorax, abdomen and pelvis identified likely pulmonary metastasis and metastasis to the left sacral lymph node, as well as the aggressive lesion in the ilial body (Figure 2). The decision was made to perform a hemipelvectomy for palliative therapy along with adjunctive I/V chemotherapy with carboplatin (DBL Carboplatin Injection; Pfizer New Zealand, Auckland, NZ) at 300 mg/m2 at 3-weekly intervals.
A left total hemipelvectomy was performed, utilising osteotomies of the pubis, ischium, and left sacrum. A sacral lymph node was also removed. Blood vessels were ligated with 2/0 PDS. No complications arose during surgery.
Histopathology of the amputated limb and hemipelvis confirmed the diagnosis of osteosarcoma. Neoplastic cells were present in the sacral tissue hence clean surgical margins were not obtained.
The dog appeared bright and comfortable after surgery and was strongly ambulatory the day of surgery. He was discharged 3 days later. The dog was still alive 13 months later, and although the dog was not restaged, no new abnormalities were detected on physical exam. Limb function, as subjectively assessed by both the owner and veterinarian, was excellent, though the dog was unwilling to jump.


Fig.2 Post-contrast computed tomography images of the pelvis of an 11-year-old Staffordshire Bull Terrier showing a large, multi-lobulated mass lesion (*) with soft tissue density and associated lysis and periosteal bone formation of the ilial body. The mass is compressing and displacing the rectum.
CASE THREE
A 9-year-old, male, neutered Cairn Terrier presented with an 8-month history of chronic, non-weightbearing lameness of the right hindlimb with severe neurogenic atrophy of the hamstring, gastrocnemius and cranial tibial muscle groups. Magnetic Resonance Imaging (MRI) identified severe, nodular, isointense thickening of the right lumbosacral trunk (Figure 3a), sciatic nerve (Figure 3b) and proximal portion of the tibial nerve where it branched at the caudal aspect of the stifle joint. The right seventh lumbar nerve root was thickened as it exited its intervertebral foramen. Samples of the nerve mass taken by ultrasound-guided fine needle aspirate and tru-cut biopsy were analysed and a malignant peripheral nerve sheath tumour (PNST) was diagnosed. Staging using CT showed no evidence of metastasis. CT the likely extension of the PNST from the sciatic nerve to the lumbosacral trunk and sixth (L6) and seventh (L7) lumbar nerve roots.
A subtotal cranial hemipelvectomy was performed with osteotomies at the ischium, pubis and right lateral wing of the sacrum to expose the sacral plexus. A right hemilaminectomy of L6 and L7 was performed to expose the spinal canal. The L6 and L7 nerve roots showed gross thickening and were transected as far proximally as possible, while the first and second sacral nerve roots appeared normal and were resected at the level of their foramina. Nerves were anaesthetised with lignocaine prior to transection. Blood vessels were ligated with 3/0 PDS.
Histopathology of the amputated limb, hemipelvis, and nerve roots revealed a poorly differentiated sarcoma (most consistent with peripheral nerve sheath tumour) that largely effaced the sciatic nerve and extended into the L7 nerve root. Polyradiculoneuritis was also present histopathologically. Surgical margins appeared clean, but with only a narrow margin of 3 mm in the L7 nerve root.
The dog recovered well from the hemipelvectomy and was able to walk well both with and without sling assistance 1 day after surgery. He was discharged 3 days after the operation. Four months after surgery, the owner subjectively scored the dog’s return to function as 9 on a 10-point scale. The dog was described as mobile, able to navigate stairs, swim, and waswalked twice daily without appearing painful. However, the owner reported a slight loss in stamina and that the dog could no longer jump upwards. Twelve months post-operatively, he was reported as happy and healthy.


Fig.3 Post-contrast sagittal magnetic resonance images of the right hindlimb of a Cairn Terrier with an 8-month history of non-weightbearing lameness showing (a) severe, nodular isointense thickening at the level of the sacral plexus (red arrows) and (b) the same nerve mass affecting the sciatic nerve and proximal tibial nerve (red arrows). a=tensor fascia latae; b=rectus femoris; c=vastus intermedius; d=adductor magnus et brevis; e=semitendinosus; f=gluteal muscles.
Table 1. Summary of presenting signs, treatment, outcome and diagnosis of three dogs that underwent hemipelvectomy for palliative treatment of peripelvic neoplasia.
DISCUSSION
Hemipelvectomy is a technically challenging, but very versatile surgical technique, with broad applications to various neoplastic conditions of the hemipelvis and its surrounding anatomy. All dogs in this study achieved either microscopic or biologic control of their local disease. That is, two dogs had clean surgical margins, while the dog with dirty surgical margins has shown no evidence of local tumour recurrence in the past 13 months. Although the dogs all had markedly different presentations and diagnoses, the one surgical modality was used effectively in all three cases.
All three dogs in this study presented with pain and severe lameness as their predominant symptoms. Therefore, the primary objective of treatment was to immediately reduce or eliminate the pain associated with their tumour. Hemipelvectomy was effective in relieving the tumour-associated pain in all three dogs, providing a high quality of life within 12–24 hours in all dogs, even in a palliative setting. Other analgesic strategies for pathologic neoplastic pain have low success and weren’t viable alternatives for these cases (Fan et al. 2007, Mathews 2008).
Hemipelvectomy was also the most appropriate oncologic treatment for these dogs, offering the best chance of survival compared to other single-modality or neoadjuvant treatments (Szewczyk et al. 2015). Osteosarcomas are highly malignant with rapid metastasis, therefore the most effective treatment is combining surgery, single agent chemotherapy and radiotherapy (Szewczyk et al. 2015). Similarly, surgery is the mainstay of treatment for peripheral nerve sheath tumours, although survival times are enhanced with adjunctive radiation therapy (Lacassagne et al. 2018). The hemipelvectomy also removed the source of the dog’s pain, providing a high quality of life, even in a palliative setting.
Owner satisfaction after the hemipelvectomy was high, as was clinical outcome and return to function. This suggests that althoughthe hemipelvectomy is an invasive procedure, it does not deserve the stigma of being a last resort, poor-outcome surgery. These findings are mirrored by a recent study that states “perioperative complications were infrequent, with patient recovery and long-term function no different than described for pelvic limb amputation” (Bray et al. 2013).
Intraoperative complications – most importantly intraoperative haemorrhage, accidental dissection of nerves, and rectal or urethral damage – are considered low risk as long as care is taken during the surgical approach and dissection (Bray et al. 2013). No complications were seen in these cases, partly due to rigorous pre-operative planning and preparation. The tumours were mapped using CT to plan the surgical approach, cross-matched fresh whole blood was ready for transfusion if required, and surgeons had clear knowledge of the relevant regional anatomy. In Case 3, resection of the first and second sacral nerve roots involved potential disruption of the right pudendal nerve. This didn’t appear to adversely affect the dog, and function of the perineal region was maintained post-operatively.
While early post-operative outcome was excellent in all cases, medium-term outcome was variable. In this study, one dog was euthanised due to tumour-related clinical progression, while the two other dogs were still alive 386 days and 379 days after surgery. Bray et al. demonstrated a median disease free interval of 49–126 days and 226 days for osteosarcoma and soft tissue sarcoma respectively, with 50% survival at 1 year (Bray et al. 2013). Multiple studies document a curiously high rate of incomplete tumour resection due to tumour size and location e.g. medial extension of PNST (Bray et al. 2013, Barbur et al. 2015). Infiltrated surgical margins reduce the time to recurrence and reduce median survival times (Lacassagne et al. 2018). In this study, the histopathologic tumour margin had no correlation to clinical or oncologic outcome. Due to the difficulty in obtaining clean surgical margins, one could question whether this invasive and expensive procedure is justifiable, especially in cases where there is already metastasis. The owner’s goals must be discussed prior to surgery. In this case study, a survival time of months to years was preferable to immediate euthanasia, the only alternative due to the degree of welfare impairment.
Based on our experience, and the clinical outcomes detailed in this study, we propose a paradigm shift involving hemipelvectomy. Rather than seeing the surgery as a radical, ‘heroic’ treatment, it should instead be considered as much for palliative therapy in cases such as these with advanced disease. While the surgery is technically challenging, and attention to perioperative patient care is paramount, hemipelvectomy patients in our experience have exceptional recoveries and return to function, with little difference to pelvic limb disarticulation (Dickerson et al. 2015). Although case reports and larger retrospective studies are still few and far between, they are increasingly recognising the role of hemipelvectomy in the treatment of a range of pelvic neoplasms (Bray et al. 2013, Ens 2017, Vinayak 2018). This novel treatment may not be novel for long.
ACKNOWLEDGEMENTS
Special thanks to Dr. Alastair Coomer and Dr. Richard Jerram at VSA for use of their cases and support in writing the report.
References:
Barbur LA, Coleman KD, Schmiedt CW, Radlinksy MG. Description of the anatomy, surgical technique, and outcome of hemipelvectomy in 4 dogs and 5 cats. Veterinary Surgery 44, 613–626, 2015
Bray JP, Worley DR, Boston SE, Romanelli G, Liptak JM, Scase TJ. Hemipelvectomy: Outcome in 84 dogs and 16 cats. A veterinary society of surgical oncology retrospective study. Veterinary Surgery 43, 27–37, 2013
Dickerson VM, Coleman KD, Ogawa M, Saba CF, Cornell KK, Radlinsky MG, Schmiedt CW. Outcomes of dogs undergoing limb amputation, owner satisfaction with limb amputation procedures, and owner perceptions regarding postsurgical adaptation: 64 cases (2005–2012). Journal of the American Veterinary Medical Association 247, 786–792, 2015
Ens MTB, Stocco MB, Gomes LG, Soares LMC, Dower NMBD, Menegassi CC, Guimarães MD, Colodel EM, de Souza RL. Total hemipelvectomy in a cat with osteoblastic osteosarcoma. Acta Scientiae Veterinariae 45, 190, 2017
Fan TM, de Lorimier LP, O’Dell-Anderson K, Lacoste HI, Charney SC. Single-agent pamidroate for palliative therapy of canine appendicular osteosarcoma bone pain. Journal of Veterinary Internal Medicine 21, 431–439, 2007
Kramer, A, Walsh, PJ, Seguin, B. Hemipelvectomy in dogs and cats: technique overview, variations, and description. Veterinary Surgery 37, 413–419, 2008
Lacassagne K, Hearon K, Berg J, Séguin B, Hoyt L, Byer B, Selmic LE. Canine spinal meningiomas and nerve sheath tumours in 34 dogs (2008–2016): distribution and long-term outcome based upon histopathology and treatment modality. Veterinary and Comparative Oncology 16, 244–351, 2018
Mathews KA. Neuropathic pain in dogs and cats: If only they could tell us if they hurt. Veterinary Clinics: Small Animal Practice 38, 1365–1414, 2008
Szewczyk M, Lechowski R, Zabielska K. What do we know about canine osteosarcoma treatment: review. Veterinary Research Communications 39, 61–67, 2015
Vinayak A, Worley DR, Withrow SJ, Adams DS, Powers BE. Dedifferentiated chondrosarcoma in the dog and cat: a case series and review of the literature. American Animal Hospital Association 54, 50–59, 2018
Author:
GRACE KAEMPER, BVScV student
Companion Quarterly: Official Newsletter of the Companion Animal Veterinarians Branch of the NZVA | Volume 31 No 2 | June 2020