 Fourteen years ago I had the privilege of meeting Ronald Tudman, a young French bulldog, and his Mum Maxelyn. The actual meeting was much more stressful because Ronald arrived in severe respiratory distress, mouth open with a large blue tongue protruding and the unforgettable noise of an incompetent larynx failing to meet requirements.
Fourteen years ago I had the privilege of meeting Ronald Tudman, a young French bulldog, and his Mum Maxelyn. The actual meeting was much more stressful because Ronald arrived in severe respiratory distress, mouth open with a large blue tongue protruding and the unforgettable noise of an incompetent larynx failing to meet requirements.
Ronald was suffering from acute laryngeal collapse secondary to brachycephalic syndrome (BS, also called brachycephalic airway syndrome or brachycephalic airway obstructive syndrome). We now know that brachycephalic syndrome is a complex disorder that includes a wide range of pathologies. The most commonly recognized are the associated respiratory problems but brachycephalic dogs and cats also suffer a range of digestive disorders, sleep disorders/apnoea, exercise and heat intolerance, dermatological and ocular conditions. It is an interesting aside that , as clinicians, we recognize that people do not seem to perceive the relevance and importance of signs such as “snoring or snuffling” , noisy breathing, regular waking ( sleep apneoa) or inability to walk more than 10 minutes in summer. A recent paper based on a questionnaire revealed that people thought this was “normal for the breed”. They only became concerned when their dog collapsed with heat stroke or had an episode of respiratory distress. This is where we as veterinary practitioners, have an ability to educate and advise new owners of brachycephalic dogs about early treatment of some of the anatomical anomalies.
 Briefly, BS consists of primary anatomic defects and secondary effects resulting from prolonged respiratory abnormalities and increased respiratory resistance. Some of the primary defects are stenotic nares, under-sized nasal chambers, malformed nasal conchae, elongated soft palate, oesophgeal deviation and hypoplastic trachea. Secondary effects include everted lateral ventricles, a spectrum of laryngeal collapse, gastrointestinal signs including reflux and vomiting and collapse of main stem bronchi. BS dogs have chronic hypoxia with reduced arterial O2 and elevated arterial CO2 and are prone to hypertension. The relationship between gastro-oesophageal reflux disease (GORD) and airway disease is much better understood in humans than in veterinary patients but BS dogs have a high incidence of gastritis and oesphagitis. Reflux is common in these patients especially post-anaesthesia/surgery.
Briefly, BS consists of primary anatomic defects and secondary effects resulting from prolonged respiratory abnormalities and increased respiratory resistance. Some of the primary defects are stenotic nares, under-sized nasal chambers, malformed nasal conchae, elongated soft palate, oesophgeal deviation and hypoplastic trachea. Secondary effects include everted lateral ventricles, a spectrum of laryngeal collapse, gastrointestinal signs including reflux and vomiting and collapse of main stem bronchi. BS dogs have chronic hypoxia with reduced arterial O2 and elevated arterial CO2 and are prone to hypertension. The relationship between gastro-oesophageal reflux disease (GORD) and airway disease is much better understood in humans than in veterinary patients but BS dogs have a high incidence of gastritis and oesphagitis. Reflux is common in these patients especially post-anaesthesia/surgery.
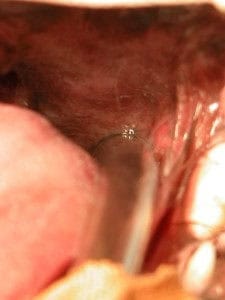
 Diagnosis involves thoracic radiology to assess tracheal diameter, evidence of cardiomegaly, pulmonary oedema, aspiration pneumonia or oesophageal deviation. Physical assessment with pharyngoscopy, laryngoscopy and possible endoscopy of the trachea and/or upper gastrointestinal tract is required to determine the primary and secondary changes. Surgical intervention can range from nasoplasty and shortening of the soft palate with resection of everted lateral ventricles to tracheostomy (temporary or permanent) or partial laryngectomy.
Diagnosis involves thoracic radiology to assess tracheal diameter, evidence of cardiomegaly, pulmonary oedema, aspiration pneumonia or oesophageal deviation. Physical assessment with pharyngoscopy, laryngoscopy and possible endoscopy of the trachea and/or upper gastrointestinal tract is required to determine the primary and secondary changes. Surgical intervention can range from nasoplasty and shortening of the soft palate with resection of everted lateral ventricles to tracheostomy (temporary or permanent) or partial laryngectomy.
Ronald had stage III laryngeal collapse – See table below.
STAGES OF LARYNGEAL COLLAPSE
Grade
Description
Stage II
Stage III
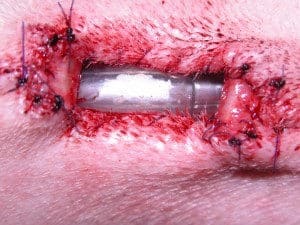
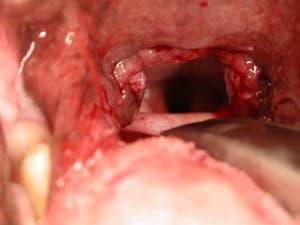
 This was confirmed under emergency anaesthesia so I could get Ronald intubated and oxygenated. The decision from there was a choice of partial laryngectomy – partial removal of one side of the rima glottidis to create a permanently “open” larynx. Usually a temporary tracheostomy is required for the first 24-48 hours to recover these patients and they have an ongoing risk of aspiration pneumonia. The other choice was permanent tracheostomy to bypass the larynx. Many brachycephalic animals are poor candidates for this procedure because of body conformation – short thick necks with excessive skin folds and small tracheal diameter. Permanent tracheostomy also requires a dedicated owner willing to go through the initial phase of excessive mucous production, regular maintenance of the tracheal stoma and the life-time management of a dog with an opening directly into the cervical trachea – obviously these guys can’t swim!
This was confirmed under emergency anaesthesia so I could get Ronald intubated and oxygenated. The decision from there was a choice of partial laryngectomy – partial removal of one side of the rima glottidis to create a permanently “open” larynx. Usually a temporary tracheostomy is required for the first 24-48 hours to recover these patients and they have an ongoing risk of aspiration pneumonia. The other choice was permanent tracheostomy to bypass the larynx. Many brachycephalic animals are poor candidates for this procedure because of body conformation – short thick necks with excessive skin folds and small tracheal diameter. Permanent tracheostomy also requires a dedicated owner willing to go through the initial phase of excessive mucous production, regular maintenance of the tracheal stoma and the life-time management of a dog with an opening directly into the cervical trachea – obviously these guys can’t swim!
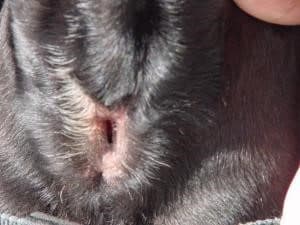
 In my assessment Ronald had a conformation appropriate for permanent tracheostomy. More importantly he had two dedicated parents who were willing to give this a go and give Ronald a chance at life. His surgery went well and he recovered without mishap – I will always remember the look on his face when he took his first breath post-surgery. It was one of disbelief that getting air could be so easy. Every breath he took, it was as though he was going to put in a great effort and suddenly the breath came without resistance. And now to see him back 14 years later with an old worn-out body is just magic. He is the oldest Frenchie I have seen and I believe it is, at least in part, because he has not had to wrestle for every breath. And, of course he had Maxelyn and Robert on his team and that is where the true acknowledgement should go. He had the best of care and love for 16 years and he has lived to be a very old boy.
In my assessment Ronald had a conformation appropriate for permanent tracheostomy. More importantly he had two dedicated parents who were willing to give this a go and give Ronald a chance at life. His surgery went well and he recovered without mishap – I will always remember the look on his face when he took his first breath post-surgery. It was one of disbelief that getting air could be so easy. Every breath he took, it was as though he was going to put in a great effort and suddenly the breath came without resistance. And now to see him back 14 years later with an old worn-out body is just magic. He is the oldest Frenchie I have seen and I believe it is, at least in part, because he has not had to wrestle for every breath. And, of course he had Maxelyn and Robert on his team and that is where the true acknowledgement should go. He had the best of care and love for 16 years and he has lived to be a very old boy.
“Patients like Ronald are what we do this job for.

DR ALEX WALKER
Alex graduated with distinction in 1978 from Massey University and spent two years in small animal practice in Auckland. In 1981 he was accepted…

